A herniated disc is a common spinal condition that affects millions of people worldwide. It occurs when the soft, jelly-like material inside a spinal disc protrudes through a tear in the outer layer of the disc, putting pressure on nearby nerves and causing pain and discomfort. In certain situations, spinal surgery for a herniated disc may be required to alleviate symptoms. Together, we will explore when spinal surgery for a herniated disc is necessary and what I do during the minimally invasive procedure, if we determine it necessary.
What Is a Herniated Disc?
The backbone is made up of small bones called vertebrae. Between these bones are soft, flexible cushions called spinal discs. These cushions help protect the spine and allow us to move around by bending, twisting, and stretching. The spinal discs act as shock absorbers and allow for movement and flexibility of the spine. A herniated disc occurs when the soft, jelly-like material inside a spinal disc protrudes through a tear in the outer layer of the disc. This can cause pressure on the spinal nerves, leading to pain, numbness, and weakness in the affected area.
Symptoms of a herniated disc may include:
- Pain in the affected area, such as the lower back or neck
- Numbness or tingling in the arms or legs
- Weakness in the affected area
- Difficulty standing, walking, or sitting
- Reduced range of motion
Spinal Surgery for Herniated Disc
Spinal surgery for a herniated disc is a treatment option that is considered when conservative treatments, such as physical therapy, medication, or chiropractic care, have failed to relieve symptoms. Spinal surgery may also be necessary if the herniated disc is causing nerve damage or bowel or bladder problems.
There are two main types of spinal surgery for a herniated disc.
Discectomy
A discectomy is a surgical procedure that involves removing the part of the herniated disc that is causing pressure on the spinal nerves. This is typically done through a small incision in the back or neck, using a microscope or special surgical instruments. The procedure is usually performed on an outpatient basis, and patients can usually return to normal activities within a few weeks.
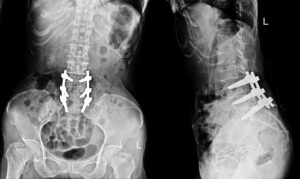
Spinal Fusion
Spinal fusion is a surgical procedure that involves fusing two or more vertebrae together to stabilize the spine. This is typically done using bone grafts, metal rods, or screws to hold the vertebrae together. Spinal fusion may be necessary if the herniated disc has caused instability in the spine or if there is a risk of further damage to the spinal nerves.
When Is Surgery Necessary?
Spinal surgery for a herniated disc is not always necessary, and conservative treatments are often effective in relieving symptoms. However, surgery may be necessary in the following cases:
Nerve Damage: If the herniated disc is causing nerve damage, spinal surgery may be necessary to relieve pressure on the nerves and prevent further damage.
Bowel or Bladder Problems: If the herniated disc is causing bowel or bladder problems, spinal surgery may be necessary to prevent permanent damage.
Chronic Pain: If conservative treatments have failed to relieve chronic pain, spinal surgery may be considered as a last resort.
Loss of Mobility: If the herniated disc is causing loss of mobility, spinal surgery may be necessary to restore mobility and quality of life.
Lack of Improvement: If conservative treatments have failed to improve symptoms after six to eight weeks, spinal surgery may be considered.
Risks and Complications of Spinal Surgery for Herniated Disc
While generally safe it carries some risks and complications. These may include:
- Infection
- Bleeding
- Nerve damage
- Spinal fluid leakage
- Blood clots
- Reaction to anesthesia
- Failure to relieve symptoms
It is essential to discuss the risks and benefits of spinal surgery with your doctor before making a decision.
Recovery and Rehabilitation After Spinal Surgery for Herniated Disc
This can vary depending on the individual case and type of surgery. Patients typically stay in the hospital for a few days after surgery to monitor for any complications. Pain medication and physical therapy are usually prescribed to manage pain and promote healing.
Physical therapy is an essential part of the recovery process. Physical therapists can provide exercises and stretches to improve strength and mobility in the affected area. They can also help patients regain proper posture and body mechanics to prevent future spinal problems.
Patients are typically advised to avoid heavy lifting and strenuous activities for several weeks after surgery to allow for proper healing. Walking and light exercise are encouraged to promote blood circulation and prevent blood clots.

Don’t Let the Pain Persist
If you are feeling any discomfort in your back, or think you may have a herniated disc, let us perform a diagnostic evaluation to determine the cause of the symptoms.
The primary goal of The Institute for Comprehensive Spine Care is to offer compassionate and convenient medical care to individuals requiring it. I am dedicated to promoting the benefits of preventive healthcare measures and utilizing minimally invasive surgical techniques whenever possible. Open communication and personalized care are a priority for all of our patients. If you are encountering spinal discomfort or a decline in your daily activities, please reach out to us to book a consultation.